The arrival of warm weather—always welcome—also marks the beginning of pollen allergy season. In Quebec, one million people suffer each year from related symptoms. This article mainly presents the results of a study conducted in 2019 by the Observatoire québécois de l’adaptation aux changements climatiques (OQACC, 2021). The survey was carried out across all regions of Quebec among 1,659 individuals aged 18 or older who reported having pollen allergies. The goal was to document the behaviours adopted by these individuals to reduce their allergy symptoms.
Situation in Quebec
In Quebec, pollen allergy season begins as soon as the snow melts, in April or May. Tree and shrub pollen predominates during this period. From May to July, it is replaced by grass pollen, such as hay and lawn grass (Canuel & Lebel, 2012). This family of pollen triggers symptoms in nearly 63% of people with pollen allergies. From late July until the first frosts in October, weed pollen appears, mainly ragweed. Ragweed pollen triggers symptoms in almost half (47%) of those allergic to pollen.
According to the OQACC survey, nearly 57% of people with pollen allergies report being allergic to at least two of the three major pollen families (trees, grasses, or weeds). As a result, symptoms may persist over a long period for many of them. Moreover, just over one in five allergic individuals (23%) report experiencing symptoms for all three pollen families present in Quebec.
Pollen allergy, commonly called “hay fever,” is an immune system reaction that occurs after exposure to a normally harmless substance, such as pollen. Histamine is released by certain immune cells—mast cells—triggering inflammation meant to protect the body from potentially harmful substances.
Symptoms of this immune response include nasal congestion and discharge, sneezing, and eye irritation.
A Link to Climate Change?
In 2014–2015, the Quebec Population Health Survey estimated that about one in seven adults (14%) experienced pollen allergy symptoms (Ministère de la Santé et des Services sociaux, 2019). With climate change, earlier springs and later first frosts are expected, which would lengthen the period during which pollen is present in the air and extend symptom duration. According to a study conducted in Montreal, the flowering period of ragweed increased from 42 days in 1994 to 63 days in 2002 (Demers, 2013). Warmer summers are also expected across Quebec, promoting the spread of certain plants like ragweed into regions where they are not yet abundant. People living in these regions—particularly those farther north—would be exposed to new allergens and could develop allergic symptoms as a result of this new exposure (Demers, 2013).
Air pollution also affects pollen allergies. For example, higher concentrations of carbon dioxide stimulate plant growth and pollen production. The population is therefore more exposed to higher concentrations of pollen and may develop pollen allergies due to sensitization. Additionally, air pollutants such as ozone, nitrogen dioxide, sulfur dioxide, carbon dioxide, and fine particles can degrade pollen structure, leading to the release of the allergens they contain. They also weaken nasal mucous membranes, making allergic individuals more sensitive to pollen (Demers, 2013).
Effects of Symptoms
Based on the definition used by the ARIA initiative, which specializes in pollen allergies and asthma (Klimek et al., 2019), OQACC study results show that slightly more than half (59%) of those with pollen allergies experience severe symptoms. Among them, 58% are bothered by nasal symptoms and 52% by eye symptoms; 40% experience sleep disturbances, 36% have trouble concentrating, 44% experience reduced productivity at work or school, and 34% are limited in daily, leisure, or sports activities.
Additionally, about 29% of individuals with severe symptoms reported feeling irritable or in a bad mood (always or often) when experiencing symptoms. Finally, 7% had to miss work or school due to their symptoms.
Treatment and Medication
Pollen allergy symptoms can be relieved in several ways, such as following immunotherapy treatment, taking medications, or limiting exposure to pollen.
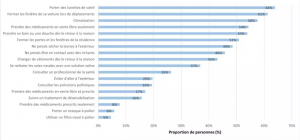
Figure 1. Proportion of people with pollen allergies who adopt behaviours to reduce their symptoms or exposure to pollen.
The most effective treatment remains immunotherapy, especially for severe allergies. It consists of regularly exposing the allergic person to small doses of allergens over several years. According to the 2019 OQACC study conducted in Quebec, 16% of respondents were undergoing immunotherapy (Figure 1), and nearly three‑quarters (71%) found it very or somewhat effective in reducing symptoms (Figure 2).
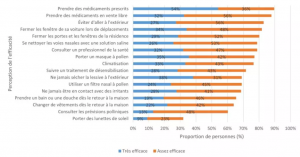
Figure 2. Figure 2. Proportion of people who perceive the behaviours they adopted as very or fairly effective.
Medication is very often used to relieve pollen allergy symptoms. About 79% of respondents in the OQACC study reported using medication. Specifically, 54% took only over‑the‑counter (OTC) medication, 8% took only prescription medication, and 17% used both (Figure 1). Among those who used prescription or OTC medication, nine out of ten found it very or fairly effective in reducing symptoms (Figure 2). Study results also show that more than three‑quarters reported that their symptoms were completely or largely relieved by medication—77% for OTC medication and 86% for prescriptions (not shown in figures).
Interestingly, among those who used both prescription and OTC medication, 89% found prescription medication very (41%) or fairly (48%) effective, compared to 78% who found OTC medication very (29%) or fairly (49%) effective. Results also indicate that those who used both types of medication reported side effects more often (38%) than those who used only OTC (23%) or only prescription medication (29%). Indeed, both OTC antihistamines and prescription medications like nasal corticosteroids can cause side effects. Antihistamines—especially first‑generation ones (e.g., Benadryl)—may cause drowsiness.
A personalized treatment plan is one advantage of consulting a healthcare provider when symptoms arise. Among the 26% who consulted a healthcare professional in the previous three years (Figure 1), about 79% felt that the visit effectively helped reduce their symptoms (Figure 2).
Reducing Exposure to Pollen
Because medication is not always effective and may cause side effects, specialists recommend that allergic individuals adopt preventive behaviours to reduce pollen exposure. These behaviours can be practiced at home or outdoors (Gouvernement du Québec, 2020). For example, it is recommended to avoid going outside when pollen concentrations are high. Despite this, OQACC study results show that only 20% of people with allergies avoided going outdoors (Figure 1).
However, strategies exist to reduce outdoor pollen exposure, such as closing car windows or wearing sunglasses, a pollen mask, or a nasal pollen filter. According to the OQACC study, wearing a mask or nasal filter is among the most effective measures. Nevertheless, although perceived by respondents as highly effective, these two behaviours were the least adopted: only 6% and 5% used a pollen mask or nasal filter, respectively (Figure 1). Yet 77% and 69% of those who used them found them very or fairly effective (Figure 2).
In contrast, although wearing sunglasses was adopted by more than half (64%) of people with pollen allergies, only 32% found them effective. While sunglasses may reduce the amount of pollen entering the eyes, their effectiveness depends on factors such as wind speed and direction. They also do not help reduce nasal symptoms.
Although specialists recommend closing doors and windows at home during times when pollen concentrations are high, only 51% of respondents did so. Ventilating the home is recommended when pollen levels are lower, such as before sunrise and after sunset. However, 20% of respondents incorrectly believed that pollen concentrations remained the same throughout the day, and 11% reported being unaware of this fact.
Showering and changing clothes immediately after being outdoors are other behaviours that reduce the amount of pollen brought into the home. These behaviours were adopted by 54% and 43% of respondents (Figure 1), and 65% and 64% found them effective (Figure 2).
Although respondents perceived them as effective, other measures adopted at home were used by less than half of respondents, including nasal saline rinsing (37%) and avoiding drying laundry outdoors during pollen season (49%). Among those who adopted these behaviours, 79% and 69% respectively found them very or fairly effective. Additionally, 46% avoided contact with other irritants (e.g., tobacco smoke, scented candles, perfume) (Figure 1), and 69% found this strategy effective (Figure 2). These substances can worsen allergy symptoms.
Finally, only 19% of participants reported checking pollen forecasts (Figure 1). Yet these forecasts help determine the best time to begin preventive behaviours. However, only three stations measure pollen concentrations in Quebec, reducing precision in some regions. Specialists also recommend consulting air pollution bulletins (such as smog warnings), as pollution episodes can worsen pollen allergy symptoms. This aspect was not measured in the OQACC survey.
Conclusion
According to the 2014–2015 Quebec Population Health Survey, nearly one in seven people had pollen allergy symptoms in Quebec. Of these, fewer than half (44%) had received a medical diagnosis. Although most people with pollen allergies use medication or adopt preventive behaviours to reduce exposure, more than half (59%) still experienced severe symptoms.
Climate change, including air pollution, will likely influence the prevalence and severity of pollen allergy symptoms. Governments and health professionals should take action now to better inform at‑risk populations about available treatments. Raising awareness of behaviours that reduce pollen exposure remains essential.
It is important to remember that the entire Quebec population—whether allergic or not—can help reduce the amount of pollen in the air. Actions include controlling ragweed growth on one’s property and avoiding planting species with allergenic pollen (e.g., birch, poplar, ash) near densely populated areas.
Source: https://climatoscope.ca/article/portrait-des-allergies-au-pollen-chez-la-population-quebecoise/